Designing Environments for Parkinson’s (Part 1)
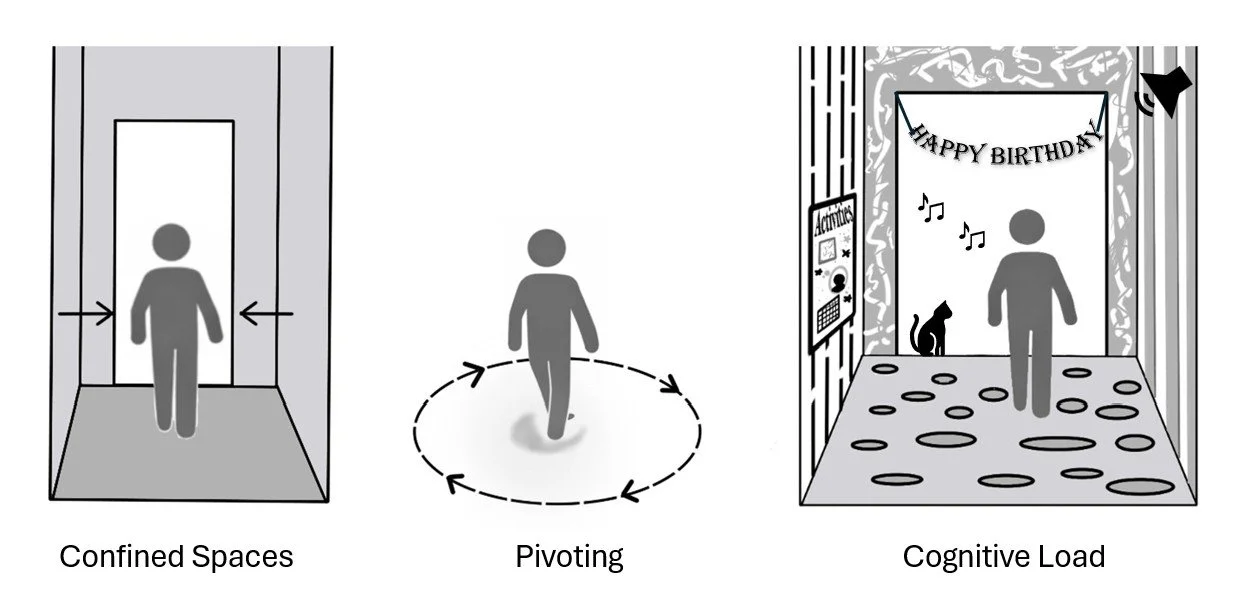
Three common triggers that cause freezing of gait (FoG) in Parkinson’s. 1. Confined spaces or narrow passages, such as doorways. 2. Pivoting or turning in place. 3. Cognitive load, visual or other sensory distractions.
How space shapes movement and daily life
According to the Parkinson’s Foundation, approximately 1.1 million people in the United States and more than 10 million people worldwide are living with Parkinson’s disease. It is the second most common neurodegenerative disease after Alzheimer’s.
Parkinson’s disease is progressive and complex. While it is often associated with movement changes, it also affects mood, cognition, and the autonomic nervous system. The loss of dopamine-producing neurons disrupts motor control, while changes in other neurotransmitter systems contribute to symptoms such as sleep disturbance, fatigue, blood pressure instability, and bladder dysfunction.
Many strategies that support people with Parkinson’s align with universal design principles, particularly those that promote intuitive use, low physical effort, perceptible information, and adequate space for approach and use. However, Parkinson’s introduces specific movement and cognitive challenges that require more targeted design responses, particularly around turning, transitions, and how movement is initiated and sustained.
Designing environments for people with Parkinson’s should focus on reducing the everyday challenges of movement by aligning the environment with how people move, think, and function.
Movement in Parkinson’s is not just slower, it is less automatic and more dependent on the environment.
This is Part 1 of a two-part series focused on design strategies that support people living with Parkinson’s.
How Parkinson’s Affects Movement
Why movement becomes less automatic and more effortful
Parkinson’s disease affects the brain’s ability to produce and regulate dopamine, a neurotransmitter that plays a key role in initiating and coordinating movement. As these systems become less effective, movement becomes slower, less automatic, and more effortful, often requiring greater attention and conscious control.
Common motor changes include:
Slowed movement
Reduced arm swing and trunk rotation
Rigidity
Changes in gait
Hesitation when turning or changing direction
Freezing of gait (FOG), where forward movement temporarily stops
These changes affect how people move through space, particularly during transitions such as turning, stopping, and starting. Some symptoms, such as freezing, may be more noticeable in certain environmental conditions, including thresholds, tight spaces, or visually complex settings.
In addition to motor changes, Parkinson’s also affects energy, attention, and sensory processing, all of which influence how easily a person can move through and respond to their environment.
Designing for Movement and Predictability
Reducing hesitation, freezing, and unnecessary effort
People with Parkinson’s often have difficulty with turning, changing direction, and adjusting their movement quickly. Spaces that require tight turns, pivoting in place, or frequent repositioning increase the likelihood of hesitation and freezing.
These challenges are not only physical. As movement requires more conscious control, it places greater demands on attention. Environments that are visually complex, cluttered, or difficult to interpret increase cognitive demand and make movement less predictable.
More supportive environments reduce these demands by allowing movement to happen gradually and with control. They support forward movement, allow time to pause and stabilize, and minimize the need for abrupt adjustments.
In practical terms, this means designing spaces that:
Allow enough open space for gradual, step-based turning rather than pivoting in place
Support clear, direct movement paths without unnecessary turns or backtracking
Minimize clutter and visual complexity, particularly near transitions such as doorways
Avoid narrow doorways, tight passages, and confined layouts that require precise movement or limit the ability to adjust position
Minimize abrupt transitions, such as thresholds or changes in flooring or lighting, that can interrupt gait or act as perceptual barriers
Provide consistent, predictable layouts so movement does not require constant adjustment
Movement challenges in Parkinson’s are not only related to strength or balance, but to how the environment is perceived and processed. Design can support movement by reducing physical, visual, and cognitive demands.
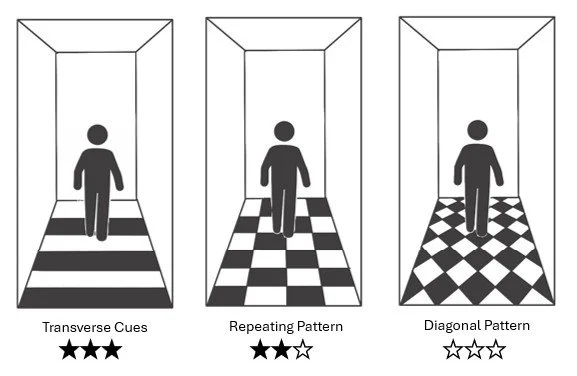
Regular, evenly spaced patterns can support gait by providing consistent visual stepping cues. Irregular or diagonal patterns are less effective. Strong contrast or certain pattern orientations may create visual illusions and should be used carefully.
Flooring
Supporting stability and how the ground is interpreted
Flooring influences both physical safety and how a space is perceived, affecting stability, confidence, and gait. For people with Parkinson’s, walking is sensitive to changes in surface conditions, particularly during turning, starting, and stopping.
Changes in flooring surfaces, such as thresholds, level changes, or transitions at doorways, can be difficult for people with Parkinson’s because they influence how the brain interprets the environment. These transitions may be perceived as barriers or obstacles, contributing to hesitation, freezing, and disrupted gait. Flooring patterns also matter. Busy, irregular, or highly contrasting designs can create visual confusion, while simple, evenly spaced repeating patterns or visual cues may support gait by providing a predictable reference for stepping.
Supportive flooring strategies include:
Providing stable, consistent surfaces that support confident foot placement
Minimizing changes in flooring materials between spaces
Ensuring transitions between flooring types are smooth and level
Avoiding busy, irregular, or highly contrasting patterns that may be misinterpreted as obstacles or changes in depth
Where visual cues are appropriate, using simple, evenly spaced repeating patterns, such as stripes or grids, to support a predictable stepping rhythm
If choosing carpet, using low-pile, firm materials that do not interfere with gait
Using compliant flooring systems that provide some shock absorption to help reduce injury from falls
Avoiding loose rugs and unsecured mats
Using slip-resistant finishes to reduce the risk of slipping
Selecting matte or low-glare surfaces to support clear visual perception
The goal is to create flooring that feels predictable underfoot and easy to interpret visually.
Visual Cues and Wayfinding
Using the environment to guide movement
People with Parkinson’s often rely on external cues to initiate and sustain movement, particularly when internal movement control is impaired. Clear, well-organized visual information can support this process.
Design strategies that support movement include:
Distinct but simple wayfinding elements
Consistent and predictable layouts
Visual targets or focal points
A focal point at the end of a corridor can act as a visual target, helping sustain forward movement and reduce hesitation by providing a clear visual destination.
At the same time, excessive visual complexity can have the opposite effect. Cluttered or visually busy environments increase cognitive load and may contribute to hesitation or freezing.
Clarity supports movement. Visual noise disrupts it.
Lighting
Shaping visibility, perception, and daily rhythm
Lighting affects movement, perception, and daily rhythm. For people with Parkinson’s, changes in lighting can alter how the environment is interpreted, influencing stability and confidence during movement.
Poor lighting can create shadows, glare, and unclear edges, all of which increase fall risk. Lighting does not only affect visibility, it influences how people move, increasing instability and the effort required to walk. Consistent, well-distributed lighting throughout a space helps reduce visual uncertainty and supports safer, more predictable movement.
Access to natural light is also important. Daylight supports visual clarity and helps regulate circadian rhythms, which are often disrupted in Parkinson’s. Exposure to brighter light during the day and softer, lower lighting in the evening can support more regular sleep and wake cycles.
Seating
Supporting safe transitions and reducing effort
Transitions such as sitting and standing are often challenging for people with Parkinson’s. Reduced motor control and impaired movement planning can lead to abrupt or uncontrolled sitting, increasing the risk of falls and injury. Seating that supports controlled, supported movement can reduce both physical strain and fall risk.
Supportive seating should be:
Firm and stable, without swivel or rocking movement
Appropriately sized, with seat heights typically around 17 to 19 inches, with some variation to accommodate different body sizes
Equipped with sturdy armrests to assist with sitting and standing
Designed with supportive backs to promote upright posture and stability
Stable under uneven pressure, so it does not tip when weight is placed on one armrest or the back
Visually distinct from the surrounding floor to improve visibility and support safe positioning before sitting
Seating should also be thoughtfully located throughout a space. Providing seating where tasks are performed, where waiting occurs, and at regular intervals along circulation routes can reduce fatigue and support safe, independent movement.
Well-designed seating supports controlled movement, not just comfort.
Acoustic and Sensory Environment
Reducing cognitive and sensory load
Parkinson’s often affects voice projection, resulting in softer or more monotone speech. At the same time, many individuals experience increased sensitivity to environmental stimuli. Acoustic and sensory conditions play an important role in communication, comfort, and the ability to engage with others.
Environments with excessive noise or reverberation can make conversation more difficult and increase the effort required to speak and process information. This added effort can contribute to fatigue and reduce participation in social interaction, which is important for maintaining connection, expressing needs, and supporting mental health.
In addition to auditory challenges, people with Parkinson’s may experience increased cognitive demand during everyday activities. Environments that are visually or acoustically complex can add to this burden, making it harder to focus, move, and respond to surroundings.
Design strategies include:
Reducing background noise and echo
Using sound-absorbing materials to support clearer communication
Minimizing visual clutter
Using cohesive, calm material palettes
Using contrast strategically to highlight transitions or important information
Reducing glare and shadows
Conclusion
Designing with movement, perception, and daily life in mind
Designing for Parkinson’s is not about eliminating challenges, but about reducing unnecessary barriers.
By supporting how movement is initiated, how environments are perceived, and how daily tasks are performed, design can help people move more safely, maintain independence, and participate more fully in everyday life.
In Part 2, I’ll apply these principles to everyday spaces, including bedrooms, bathrooms, and kitchens, to show how thoughtful design can support daily routines in practical ways.
References and Further Reading
Bhidayasiri, R., Jitkritsadakul, O., Sringean, J., Jantanapornchai, T., Kantachadvanich, N., Phumphid, S., Boonpang, K., Pensook, S., Aungkab, N., Hattori, N., & Chaudhuri, K. R. (2018). Exploring Bedroom Usability and Accessibility in Parkinson’s Disease (PD): The Utility of a PD Home Safety Questionnaire and Implications for Adaptations. Frontiers in Neurology, 9, 360.https://doi.org/10.3389/fneur.2018.00360
Cockx, H. M., Lemmen, E. M., van Wezel, R. J. A., & Cameron, I. G. M. (2023). The effect of doorway characteristics on freezing of gait in Parkinson’s disease. Frontiers in Neurology, 14.https://doi.org/10.3389/fneur.2023.1265409
Gál, O., Poláková, K., Hoskovcová, M., Tomandl, J., Čapek, V., Berka, R., Brožová, H., Šestáková, I., & Růžička, E. (2019). Pavement patterns can be designed to improve gait in Parkinson’s disease patients. Movement Disorders: Official Journal of the Movement Disorder Society, 34(12), 1831–1838.https://doi.org/10.1002/mds.27831
Hanson, J. (2022, May 29). Setting Up Your Home Environment to Live Well with Parkinson’s—Part 2. Davis Phinney Foundation.https://davisphinneyfoundation.org/blog/draft2-setting-up-your-home-environment-to-live-well-with-parkinsons-part-2/
Hesam Shariati, F., Steffens, A., & Adhami, S. (2023). Designing environments that contribute to a reduction in the progression of Parkinson’s disease; a literature review. Health & Place, 83, 103105.https://doi.org/10.1016/j.healthplace.2023.103105
Hu, Z.-D., Zhu, S.-G., Huang, J.-F., Chen, J.-Y., Huang, S.-S., Liu, R.-P., Chen, Z.-L., Ma, L.-L., Zhang, X., & Wang, J.-Y. (2023). Carpets with visual cues can improve gait in Parkinson’s disease patients: May be independent of executive function. European Journal of Medical Research, 28(1), 530.https://doi.org/10.1186/s40001-023-01472-1
Kesler, A., Leibovich, G., Herman, T., Gruendlinger, L., Giladi, N., & Hausdorff, J. M. (2005). Shedding light on walking in the dark: The effects of reduced lighting on the gait of older adults with a higher-level gait disorder and controls. Journal of NeuroEngineering and Rehabilitation, 2(1), 27.https://doi.org/10.1186/1743-0003-2-27
McNaney, R., Balaam, M., Holden, A., Schofield, G., Jackson, D., Webster, M., Galna, B., Barry, G., Rochester, L., & Olivier, P. (2015). Designing for and with People with Parkinson’s: A Focus on Exergaming. Proceedings of the 33rd Annual ACM Conference on Human Factors in Computing Systems, CHI ’15, 501–510.https://doi.org/10.1145/2702123.2702310
Parkinson’s Foundation. (2021). Parkinson’s Outcomes Project: Improving the Lives of People Living with Parkinson’s Through Research [Foundation Report].https://www.parkinson.org/Outcomes
Pokharel, A., Tamrakar, A., & Chopra, N. (2026). Use of AR/VR for Treatment of Freezing of Gait (FoG) in Parkinson’s Disease (PD). Journal of Clinical Medicine, 15(5), 2076.https://doi.org/10.3390/jcm15052076
Ramos, J. B., Duarte, G. S., Bouça-Machado, R., Fabbri, M., Mestre, T. A., Costa, J., Ramos, T. B., & Ferreira, J. J. (n.d.). The Role of Architecture and Design in the Management of Parkinson’s Disease: A Systematic Review. Journal of Parkinson’s Disease, 10(4), 1301–1314.https://doi.org/10.3233/JPD-202035
Yoo, A. S., Wise, A., Ortega, R. A., Raymond, D., Plitnick, B., Brons, J., Liang, J., Bressman, S. B., Yang, M., Pedler, D., Figueiro, M. G., & Saunders-Pullman, R. (2024). Supplemental Ambient Lighting Intervention to Improve Sleep in Parkinson’s disease: A Pilot Trial. Parkinsonism & Related Disorders, 129, 107149.https://doi.org/10.1016/j.parkreldis.2024.107149